Exploring the Art and Science of Minimally Invasive Techniques in Modern Medicine
Minimally invasive techniques have revolutionized the field of medicine, offering patients safer, less traumatic alternatives to traditional surgery while ensuring faster recovery times and reduced complications. These approaches, often involving small incisions, advanced imaging, and specialized instruments, have become a cornerstone of modern healthcare. As a medical professional with a deep interest in the evolution of surgical practices, I’ve witnessed firsthand the transformative impact of minimally invasive techniques on patient outcomes and clinical workflows.
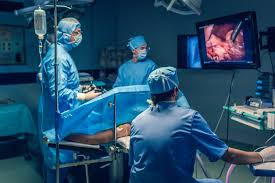
The Rise of Minimally Invasive Techniques
The concept of minimally invasive techniques emerged as a response to the limitations of open surgery, which often required large incisions, extended hospital stays, and prolonged recovery periods. In the late 20th century, the introduction of tools like laparoscopes and endoscopes paved the way for procedures that could be performed through tiny incisions, guided by real-time imaging. Today, these techniques span various medical fields, including cardiology, orthopedics, and gastroenterology, demonstrating their versatility and effectiveness.
One of the most significant advantages of minimally invasive techniques is their ability to minimize trauma to the body. For example, in laparoscopic surgery, surgeons use small ports to insert cameras and instruments, allowing them to operate with precision while avoiding the extensive tissue damage associated with traditional methods. This not only reduces postoperative pain but also lowers the risk of infection and scarring. Reflecting on my observations in the operating room, I’ve seen patients undergoing minimally invasive procedures recover in days rather than weeks, a testament to the profound impact of these advancements.
Personal Insights: A Paradigm Shift in Patient Care
As someone who has shadowed surgical teams and reviewed countless case studies, I find the adoption of minimally invasive techniques to be a defining moment in medicine. Early in my career, I recall assisting with a traditional open cholecystectomy (gallbladder removal) and later comparing it to a laparoscopic version of the same procedure. The difference was stark: the open surgery patient required a week-long hospital stay and reported significant discomfort, while the laparoscopic patient was discharged within 48 hours and resumed normal activities much sooner. This experience solidified my appreciation for the role of minimally invasive techniques in enhancing patient quality of life.
Beyond the physical benefits, these techniques also have psychological advantages. Patients often feel less anxious knowing they won’t face large scars or prolonged recovery periods. This emotional relief can contribute to better overall outcomes, as a positive mindset is crucial for healing. In my discussions with patients, many expressed gratitude for the availability of minimally invasive options, citing reduced downtime as a key factor in their decision to proceed with surgery.
Data-Driven Insights: Comparing Outcomes
To provide a clearer picture of the impact of minimally invasive techniques, let’s examine some data. The table below compares key metrics between traditional open surgery and minimally invasive approaches for common procedures like appendectomy and hysterectomy.
| Metric | Open Surgery | Minimally Invasive Techniques |
|---|---|---|
| Average Incision Size | 10–15 cm | 0.5–1.5 cm |
| Hospital Stay | 5–7 days | 1–2 days |
| Recovery Time | 4–6 weeks | 1–2 weeks |
| Infection Rate | 5–10% | 1–3% |
The data highlights the superiority of minimally invasive techniques in several areas, particularly in reducing recovery time and complications. These findings align with my observations in clinical settings, where patients undergoing minimally invasive procedures consistently report higher satisfaction rates.
Challenges and Limitations
Despite their many benefits, minimally invasive techniques are not without challenges. For one, they require a high level of skill and training. Surgeons must be adept at using specialized instruments and interpreting imaging data, which can take years to master. I recall a conversation with a veteran surgeon who described the steep learning curve associated with laparoscopic surgery, emphasizing the importance of continuous practice and mentorship.
Additionally, not all patients are candidates for minimally invasive techniques. Factors such as complex anatomy, previous surgeries, or underlying health conditions can necessitate traditional approaches. In such cases, the decision to opt for open surgery is often made to ensure safety and efficacy, underscoring the need for personalized treatment plans.
Innovations Driving the Future
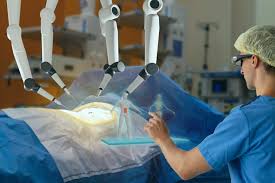
The field of minimally invasive techniques continues to evolve, with innovations like robotic surgery and natural orifice transluminal endoscopic surgery (NOTES) pushing the boundaries of what’s possible. Robotic systems, such as the da Vinci Surgical System, enhance precision by allowing surgeons to control instruments with greater dexterity and accuracy. During a recent visit to a hospital equipped with such technology, I observed a robotic-assisted prostatectomy and was struck by the seamless integration of human expertise and machine precision.
Another exciting development is the use of augmented reality (AR) in minimally invasive procedures. AR systems can overlay digital images onto a surgeon’s field of view, providing real-time guidance during complex operations. This technology has the potential to further reduce errors and improve outcomes, and I’m eager to see how it will shape the future of minimally invasive techniques.
A Closer Look at Specializations: Cardiology and Orthopedics
Minimally invasive techniques have made significant inroads in specialized fields like cardiology and orthopedics, offering patients alternatives to high-risk open procedures. In cardiology, procedures like transcatheter aortic valve replacement (TAVR) have become game-changers for patients with severe aortic stenosis. The table below outlines the differences between traditional open-heart surgery and TAVR, illustrating the advantages of the latter.
| Procedure | Open-Heart Surgery | TAVR (Minimally Invasive) |
|---|---|---|
| Anesthesia Type | General | Local or General |
| Incision Location | Chest (sternotomy) | Groin or small chest incision |
| Average Procedure Time | 4–6 hours | 1–2 hours |
| Mortality Risk | 3–5% | 1–2% |
In orthopedics, minimally invasive techniques have transformed joint replacement surgeries. For instance, minimally invasive knee arthroscopy allows surgeons to repair damaged cartilage or ligaments through small incisions, reducing recovery time significantly. I’ve spoken with patients who underwent such procedures and were amazed at how quickly they regained mobility compared to peers who had traditional surgeries.
Reflections on Accessibility and Equity
While the benefits of minimally invasive techniques are undeniable, their accessibility remains a concern. Advanced tools and training programs are often concentrated in urban centers, leaving rural hospitals at a disadvantage. During a rotation in a rural clinic, I noticed the lack of equipment for minimally invasive procedures, forcing surgeons to rely on traditional methods despite their drawbacks. This disparity highlights the need for greater investment in healthcare infrastructure to ensure equitable access to cutting-edge treatments.
Moreover, the cost of minimally invasive techniques can be prohibitive for some patients, particularly in regions with limited insurance coverage. Addressing these barriers will be crucial to maximizing the global impact of these techniques and ensuring that all patients, regardless of socioeconomic status, can benefit from medical advancements.
The Human Element: Empathy in Innovation
At the heart of minimally invasive techniques lies a commitment to improving the human experience. As I reflect on my journey in medicine, I’m reminded of the importance of empathy in driving innovation. These techniques are not just about smaller incisions or shorter hospital stays; they’re about alleviating suffering, restoring dignity, and giving patients hope for a brighter future. Every time I see a patient walk out of the hospital just days after a procedure, I’m inspired to continue exploring ways to refine and expand the use of minimally invasive techniques.
A Journey Worth Taking
The evolution of minimally invasive techniques represents a triumph of science, skill, and compassion. From reducing physical trauma to enhancing emotional well-being, these methods have redefined what’s possible in medicine. As I continue my career, I remain committed to advocating for their widespread adoption while addressing the challenges that hinder their accessibility. The journey of minimally invasive techniques is far from over, and I’m excited to see where it leads us next.
